Experiencing a positive pregnancy test is a monumental milestone on the IVF journey. However, for many, this joy is tragically short-lived, replaced by the confusion and heartache of a chemical pregnancy and IVF. Also known as a biochemical pregnancy or very early pregnancy loss, this event is a deeply emotional and often misunderstood outcome of the IVF process.
This article serves as a comprehensive guide to understanding what a chemical pregnancy is, exploring why it happens, providing support for the grief that follows, and outlining the next steps you can take with your medical team.
1. Understanding the Medical Reality of a Chemical Pregnancy
What is a Chemical Pregnancy in IVF?
A chemical pregnancy occurs when a fertilized egg implants in the uterus and begins to release hCG levels IVF—the hormone detected by pregnancy tests—but does not develop into a clinical pregnancy. Doctors use the Beta hCG test to confirm these early pregnancies.
For many women, the first sign is a positive pregnancy test then period a few days later, often heavier than usual. This is why some call it a preclinical abortion, since it ends before an embryo can be seen on an ultrasound.
When comparing chemical pregnancy vs miscarriage, the key difference is timing. A miscarriage generally happens later, after a gestational sac or embryo is visible. A chemical pregnancy is an earlier form of loss, sometimes referred to as an early miscarriage IVF.
The Anatomy of an Early Loss
In IVF, the process begins with embryo transfer, where a carefully selected embryo is placed in the uterus. A chemical pregnancy occurs when the embryo begins to implant in the uterine lining but cannot continue developing. This is considered an implantation failure rather than a later pregnancy issue.
2. Exploring the Causes Behind a Chemical Pregnancy in IVF
Embryo Quality and Chromosomal Factors
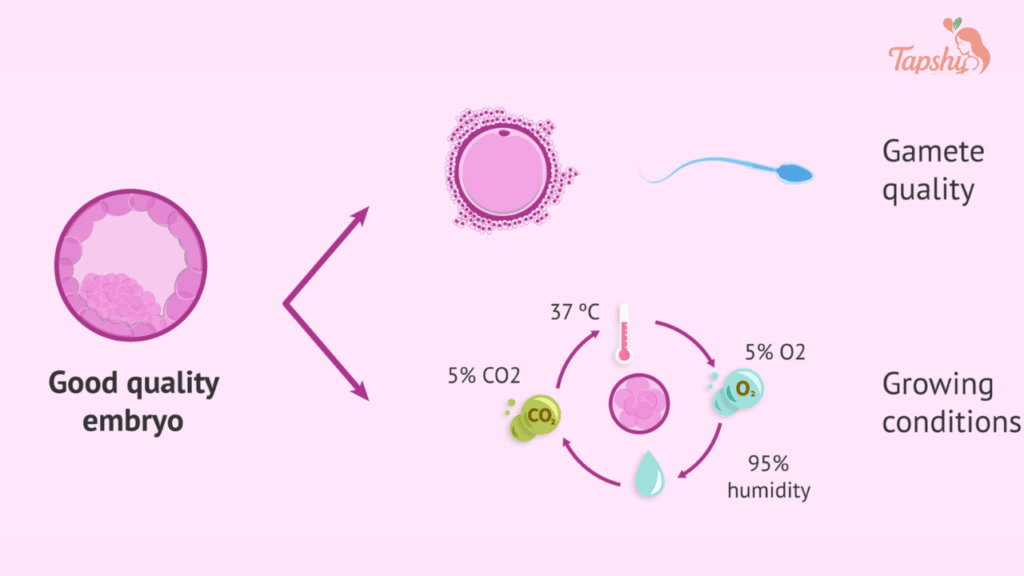
The most common explanation for why do chemical pregnancies happen in IVF lies in chromosomal abnormalities IVF. When an embryo has an incorrect number of chromosomes, it is unlikely to progress, leading to an early loss.
Embryo quality and chemical pregnancy outcomes are closely linked. Poorer quality embryos are more likely to result in early loss. One tool to address this is Preimplantation Genetic Testing (PGT-A), which screens embryos for chromosomal abnormalities before transfer.
Hormonal and Uterine Issues
Another crucial factor is progesterone levels IVF. Progesterone supports the uterine lining and helps maintain early pregnancy. If levels are low, even progesterone supplementation may be required to reduce the risk of loss.
Uterine lining issues—such as thin or irregular lining—can also prevent healthy implantation.
Other Contributing Factors
Sometimes, the reasons are less straightforward. Immunological factors IVF or blood clotting disorders can interfere with implantation. When multiple chemical pregnancies occur, doctors may diagnose Recurrent Implantation Failure (RIF) and recommend further testing.
3. The Emotional Rollercoaster and the Path to Healing
Processing Grief and Seeking Support
Even though it happens early, a chemical pregnancy carries real emotional weight. Many women describe the emotional rollercoaster of IVF—the joy of seeing that positive test followed by the devastation of loss.
It’s important to acknowledge chemical pregnancy grief. Whether you’ve been through multiple IVF rounds or this was your first, the loss is valid. Seeking chemical pregnancy support from counselors, support groups, or friends can help. Reading IVF chemical pregnancy stories can also provide comfort and remind you that you are not alone.
Finding Hope and Perspective
While devastating, many doctors reassure patients that a chemical pregnancy means implantation can occur. This often raises the question: is chemical pregnancy a good sign for IVF? The answer is yes, in some cases—it shows that the embryo and uterus did interact.
Holding onto chemical pregnancy hope may help you see this as a step forward. Your body demonstrated the ability to conceive, and many women go on to have successful pregnancies afterward.
4. Next Steps: Planning for Your Next IVF Cycle
Medical Review and Protocol Changes
After loss, your doctor will review the next steps after chemical pregnancy IVF. They may suggest adjustments such as IVF protocol changes after loss or further evaluation.
Tests like the ERA test for recurrent implantation failure can provide insights into the best timing for embryo transfer.
Considering Future Embryo Transfers
Many women proceed with a frozen embryo transfer after chemical pregnancy. This allows your doctor to make targeted changes, such as incorporating Assisted Hatching, Intralipid therapy, or a low-dose aspirin protocol to improve implantation chances.
For those with multiple losses, testing after recurrent chemical pregnancies can uncover hidden issues and guide personalized treatment.
Conclusion
A chemical pregnancy and IVF can be an incredibly painful and disheartening experience, casting a shadow over the hopeful journey of infertility treatments. However, it is also a common event that provides valuable information to your medical team.
By understanding the causes, allowing yourself to grieve, and working with your doctor to adjust your plan, you can move forward with renewed strength. Experiencing this type of loss does not mean your dream of motherhood is over—it is one step, however difficult, on the road to parenthood.
Have you experienced a chemical pregnancy? Share your story or coping strategies in the comments to help others feel seen and supported.
FAQ Section
1. How common is chemical pregnancy with IVF?
Chemical pregnancies are relatively common in IVF, accounting for a significant portion of early losses.
2. Can you prevent a chemical pregnancy?
Complete prevention isn’t always possible, but steps such as Preimplantation Genetic Testing (PGT-A), proper progesterone supplementation, and thorough screening can lower risks.
3. What are the typical symptoms of a chemical pregnancy after IVF?
Common signs include a positive hCG levels IVF test, followed by bleeding resembling a period and no pregnancy development on ultrasound.
4. What is the IVF success rates after chemical pregnancy?
Research shows that experiencing a chemical pregnancy does not decrease long-term success rates. In fact, many women achieve healthy pregnancies afterward.
5. How does a chemical pregnancy differ from a blighted ovum?
A blighted ovum involves a gestational sac forming without an embryo. A chemical pregnancy occurs even earlier, before any sac is visible.
6. Does a chemical pregnancy count as a miscarriage?
Yes, it is medically classified as a preclinical abortion, meaning it is considered an early form of miscarriage.

